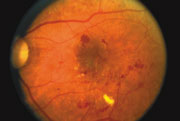
Diabetes can affect your vision. If you have diabetes, your body does not use and store sugar properly. High blood sugar levels can damage blood vessels in the retina. The damage to retinal vessels is knows as diabetic retinopathy.
DIAGNOSIS OF DIABETIC RETINOPATHY
A complete eye exam is the best way to detect changes in the eye. An ophthalmologist can often diagnose and treat serious retinopathy before you are aware of any vision problems. The physician will dilate your pupils and look inside of the eye with special equipment and lenses. If the physician finds diabetic retinopathy, a special test called a fluorescein angiography may be done to find out of you need treatment.
TREATMENT OF DIABETIC RETINOPATHY
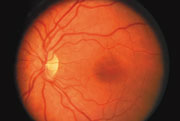
The best treatment is to prevent the development of retinopathy. Strict control of your blood sugar will reduce the long-term risk of vision loss from diabetic retinopathy.
Medical Treatment
Injections of anti-VEGF medication in the eye can stop he growth of new blood vessels and subsequent bleeding. VEGF is necessary for the eye to build new blood vessels and the use of anti-VEGF medication causes regression of these fragile and abnormal blood vessels. At times, a steroid medication may also be used.
Laser Surgery
Laser surgery is usually recommended for patients with macular edema, PDR and neovascular glaucoma. For macular edema, the laser is focused on the damaged retina near the macula to decrease the fluid leakage. The main goal of this treatment is to prevent further loss of vision. For PDR, the laser is focused on all parts of the retina except the macula. This treatment causes abnormal new vessels to shrink and often prevents them from growing. It also decreases the chance of vitreous bleeding or retinal distortion. Multiple laser treatments over time may be necessary. Laser surgery does not cure diabetic retinopathy and may not always prevent further loss of vision.
Vitrectomy
In advanced PDR, your physician may recommend a vitrectomy. This is a micro-surgical procedure in which the blood filled vitreous is removed and replaced with clear solution. Vitrectomy often prevents further bleeding by removing the abnormal vessels, which caused the bleeding. If the retina is detached, it can be repaired during the surgery. Surgery should be done early because macular distortion or traction retinal detachment will cause permanent vision loss. The longer the macula is distorted or out of place, the more serious the vision loss will be.
VISION LOSS IS PREVENTABLE
With improved methods of diagnosis and treatment, a smaller percentage of diabetics who develop retinopathy have serious vision problems. Early detection of diabetic retinopathy is the best protection against vision loss. You can lower your risk of vision loss greatly by maintaining strict control of your blood sugar and blood pressure, and by having regular check-ups with your ophthalmologist.
WHEN TO SCHEDULE AN EXAMINATION WITH AN OPHTHALMOLOGIST
Patients with Type 1 diabetes should schedule an exam within five years of being diagnosed and then yearly. Patients with Type 2 diabetes should have an exam at the time of the diabetes diagnosis and then once a year. Pregnant diabetic women should schedule and exam in the first trimester because retinopathy can progress quickly during pregnancy.
Lauderdale Eye Specialists provides this on-line information for educational purposes only and it should not be construed as personal medical advice. Lauderdale Eye Specialists disclaims any & all liability for injury or other damages that could result from use of the information obtained from this site.


